When welcoming a newborn into the world, parents are often faced with a myriad of decisions that can impact their child’s health and well-being. One such consideration is the presence of a lip tie, a common oral anomaly that can affect feeding and even speech development. Lip ties occur when the tissue connecting the upper lip to the gums is unusually tight or thick, potentially causing breastfeeding difficulties and other issues. As parents seek the best path forward, they are confronted with the choice between surgical and non-surgical options for treating lip ties. Understanding the benefits and drawbacks of each approach is essential for making an informed decision that prioritizes the child’s comfort and overall health.
What is a Lip Tie?
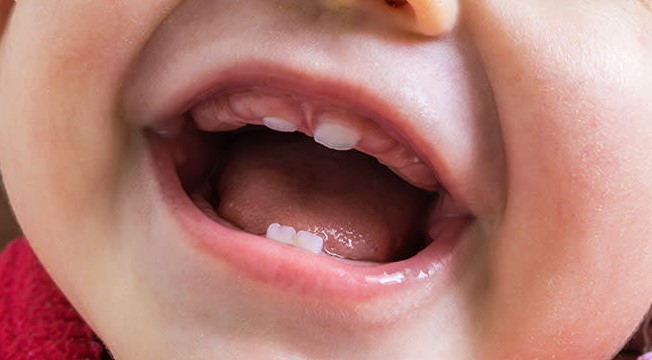
A lip tie, medically known as a maxillary labial frenulum, is a condition where the tissue connecting the upper lip and gums is tighter or thicker than usual. This can result in restricted movement of the upper lip, which can affect breastfeeding, bottle feeding, and even lead to potential speech difficulties as the child grows. The degree of severity varies, and not all lip ties require intervention. However, in cases where the tie is causing problems, parents are often faced with the choice of how to address the issue.
Non-Surgical Approaches:
1. Latch Techniques and Breastfeeding Support:
In mild cases, where the lip tie does not significantly hinder feeding, lactation consultants and healthcare providers may recommend specific latch techniques that can help improve breastfeeding efficiency. These techniques aim to compensate for the limited lip movement caused by the lip tie. Breastfeeding support can be particularly beneficial in these situations, as proper latching can alleviate many feeding challenges associated with lip ties.
2. Stretching Exercises:
Some healthcare professionals advocate for stretching exercises as a non-invasive approach to address mild lip ties. This involves gently massaging and stretching the frenulum multiple times a day. While this method does not entirely eliminate the lip tie, it can help prevent further complications and improve the range of motion of the lip.
Surgical Options:
1. Frenotomy:
A frenotomy is a minor surgical procedure that involves using sterile scissors or a laser to cut the tight or thick tissue of the lip tie. This procedure is relatively quick and can often be performed in the healthcare provider’s office. Frenotomy is recommended for cases where the lip tie is causing significant feeding problems. It is generally well-tolerated by infants and has a quick recovery period.
2. Frenuloplasty:
In cases where the lip tie is more severe or where the frenulum extends further down the gums, a frenuloplasty may be recommended. This procedure is more involved than a frenotomy and may require the use of local anesthesia. During a frenuloplasty, the surgeon will make a more extensive incision to release the tension in the tissue. This option is usually considered when other interventions have not yielded the desired results.
Making the Decision:
Choosing between surgical and non-surgical options for treating lip ties involves considering various factors, including the severity of the lip tie, the age of the child, and the potential impact on feeding and speech development. Parents are encouraged to work closely with their healthcare providers, especially those experienced in pediatric dentistry or oral surgery, to determine the most appropriate course of action.
Benefits of Non-Surgical Approaches:
1. Less Invasive:
Non-surgical options, such as latch techniques and stretching exercises, are minimally invasive and do not involve any incisions or anesthesia.
2. Low Risk of Complications:
Non-surgical approaches generally have a lower risk of complications compared to surgical procedures, making them a safer choice for some parents.
Drawbacks of Non-Surgical Approaches:
1. Limited Effectiveness:
Non-surgical methods may not be as effective for severe cases of lip ties. If the lip tie significantly impairs feeding, surgical intervention might be necessary.
2. Longer Timeline:
Achieving results with non-surgical methods might take longer than surgical procedures. If quick resolution is a priority, surgical options might be more suitable.
Benefits of Surgical Approaches:
1. Immediate Resolution:
Surgical procedures offer a swift resolution to the issue, which can be especially important for infants struggling with feeding difficulties.
2. Effective for Severe Cases:
Surgical options are often more effective for severe lip ties that substantially impact the child’s ability to breastfeed or bottle-feed.
Drawbacks of Surgical Approaches:
1. Risk of Discomfort:
Surgical procedures can cause some discomfort for the infant during and after the intervention. However, this discomfort is usually temporary.
2. Possible Anesthesia Use:
In some cases, surgical procedures might require the use of local anesthesia, which comes with its own set of considerations and potential risks.
Conclusion:
The decision to treat a lip tie in a newborn is a crucial one that requires careful consideration. While non-surgical options can be effective for mild cases, severe lip ties that hinder feeding and speech development might necessitate surgical intervention. Ultimately, the choice between surgical and non-surgical approaches should be made in consultation with qualified healthcare professionals who can assess the individual case and recommend the best course of action. The well-being of the child, along with their long-term comfort and development, should guide this important decision-making process.