Welcome to pearly whites dentists! We are a family-owned and operated dental practice that has been providing quality dental care for over 20 years. Our team of experienced dentists and hygienists are dedicated to providing the highest quality of care to our patients. We strive to make sure that each patient receives the best possible treatment and care. Our goal is to help you achieve a brighter, healthier smile. We offer a wide range of services, from preventive care to cosmetic dentistry, to help you achieve the smile you desire. We look forward to helping you achieve a brighter, healthier smile.
How Pearly Whites Dentists Can Help You Achieve a Brighter Smile
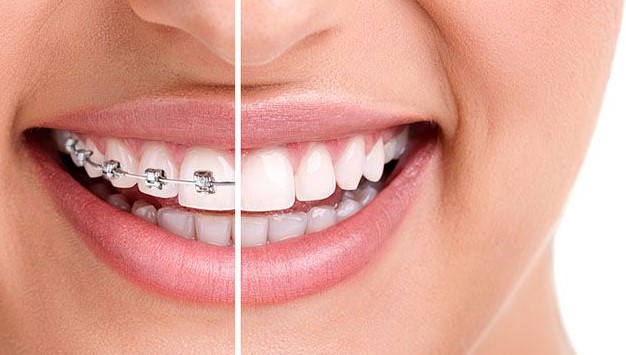
Having a bright, white smile can be a great confidence booster and can make a lasting impression on those around you. Fortunately, pearly whites dentists can help you achieve a brighter smile.
At pearly whites dentists, we offer a variety of services to help you achieve a brighter smile. Our professional teeth whitening services can help you remove years of staining and discoloration from your teeth. We use a special whitening gel that is applied to your teeth and then activated with a special light. This process can help you achieve a brighter, whiter smile in just one visit.
In addition to our professional teeth whitening services, we also offer a variety of other services to help you achieve a brighter smile. We offer dental veneers, which are thin shells that are placed over your teeth to cover up any discoloration or staining. We also offer dental bonding, which is a process that uses a special resin to fill in any gaps or chips in your teeth.
At pearly whites dentists, we understand that having a brighter smile can be a great confidence booster. That’s why we strive to provide the highest quality of care and the best results possible. Our experienced team of dentists and hygienists will work with you to create a personalized treatment plan that is tailored to your individual needs.
If you’re looking for a brighter, whiter smile, pearly whites dentists can help. Contact us today to learn more about our services and to schedule an appointment.
The Benefits of Quality Dental Care from Pearly Whites Dentists
Good dental care is essential for maintaining a healthy mouth and a beautiful smile. At pearly whites dentists, we understand the importance of quality dental care and strive to provide our patients with the best possible service. Here are some of the benefits of choosing pearly whites dentists for your dental care needs:
1. Comprehensive Care: Our team of experienced dentists and hygienists provide comprehensive care, from routine check-ups and cleanings to more complex procedures such as root canals and crowns. We also offer cosmetic dentistry services to help you achieve the smile of your dreams.
2. Advanced Technology: We use the latest technology to ensure that our patients receive the highest quality care. Our digital x-rays and intraoral cameras allow us to diagnose and treat problems quickly and accurately.
3. Comfort and Convenience: We understand that visiting the dentist can be a stressful experience, so we strive to make our office as comfortable and convenient as possible. Our friendly staff will make sure that you feel at ease during your visit.
4. Affordable Prices: We offer competitive prices for all of our services, so you can be sure that you are getting the best value for your money.
At pearly whites dentists, we are committed to providing our patients with the highest quality dental care. We believe that everyone deserves to have a healthy, beautiful smile, and we are dedicated to helping you achieve that goal. Contact us today to learn more about how we can help you maintain your oral health.
Conclusion
pearly whites dentists is a great choice for anyone looking for quality dental care and a brighter smile. Their experienced and knowledgeable staff provide a wide range of services, from routine check-ups to more complex procedures. They use the latest technology and techniques to ensure that their patients receive the best possible care. With their commitment to providing excellent customer service and a friendly atmosphere, pearly whites dentists is the perfect choice for anyone looking for a reliable and trustworthy dental care provider.